Semen analysis is a scientific examination of semen fluid to investigate male infertility or effectiveness of vasectomy procedure. The accuracy of the semen analysis might be affected by individual variables, environmental and physiological factors.
Two or more separate sperm analysis are to be done within 2-3 weeks interval. If the first sperm test result is found to be abnormal, patients are to take another test. A man could not be diagnosed as infertile as long there are live sperm in the semen.
What you should know about providing a proper semen sample
- 2-3 days before collection of the sperm, abstain from sexual intercourse or masturbation.
- Avoid caffeine, alcohol and marijuana for at least 3 months before the sperm analysis.
- Inform the doctor if you are taking any medications or any herbal remedies.
- Collection of sperm through masturbation is preferred.
- If it is against the practice of your religion, you may collect the sperm using a special type condom during sexual intercourse.
- Do not use lubricant, soap or perfume during sample collection.
- Most preferably, collect the specimen in a private room in the healthcare office.
- The sample must be delivered to the lab within one hour after ejaculation.
- If the patient collects the sample at home, remember to keep it in room temperature and bring it to the lab as soon as possible.
- Avoid providing sample when you are unwell or stressed.
What do the semen analysis results mean?
| Semen Characteristic | Reference Value |
|---|---|
| Volume (ml) | 1.5 |
| Vitality (% live) | 58 |
| Concentration (106/ml) | 15 |
| Total Sperm Count (106) | 15 |
| Motility (Progressive) % | 32 |
| Total Motile % | 40 |
| Normal Morphology (%) | 4 |
Nice.Org.UK World Health Organisation 2010
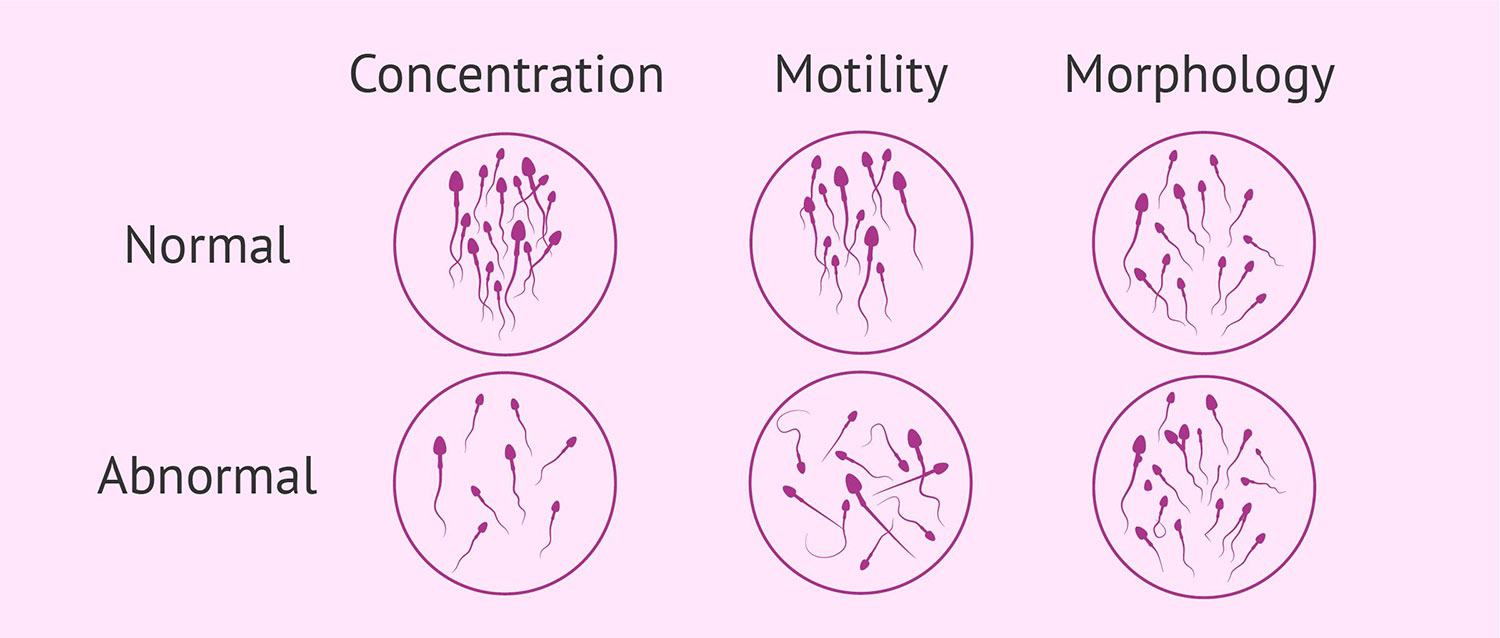
Semen Analysis Characteristics Explained:
- Volume – measures the volume of the submitted semen sample.
The minimum volume should be greater than 1.5 ml or at least half a teaspoon. For volume less than this, it might be indicative of a block in the sperm duct or a semen collection problem. On the other hand, excess fluid indicates the amount of sperm diluted or inflammation in the reproductive system.
- Sperm count- number of sperm per milliliter.
The sperm count should be at least 15 million/ml. Anything less than this indicates a low sperm count.
- Sperm movement- also known as sperm motility, measures the % of active sperm showing efficient movement. A low motility measure equates to a reduced sperm capacity to move through the female reproductive system to fertilize the egg.
At least 40% of the sperm should be demonstrating motility.
Progressive motility specifies motile sperm that moves forwards in a straight line or large circles, whereas non-progressive motile sperm are more likely to move in tight circles. At least 32% of the sperm should be demonstrating progressive motility.
- Sperm shape- also known as the morphology, measures % of normal-sized and shaped sperm. Normal sperm have a long tail and oval-shaped head. Abnormal-sized or shaped sperm can have difficulty reaching, penetrating, and fertilizing the egg.
The usual range is 4-14% sperm with standard form. You want at least 4% of sperm to be of normal shape, otherwise, you could have fertility issues because of sperm morphology.
- White blood cells – the presence of white blood cells in semen specimens indicates signs of infection.

To learn more details about the entire process, please check out KLF website Male Infertility Investigation on normal sperm count and other parameters involved in a semen analysis.
Why is sperm analysis done?
- To assess the fertility status based on sperm characteristics
- Post vasectomy check for the success of the vasectomy procedure. (Procedure is successful only if no sperm is found)
How can you improve your sperm quality?
- Avoid alcohol intake
- Stop smoking
- Stay away from high-temperature places such as spas, thermal baths, and saunas.
- Avoid tight underwear or jeans
- Complete antibiotic course prescribed by the doctor if you have white blood cells in your semen.
- Take supplements such as vitamin E or zinc.
If your sperm analysis results appear abnormal, the doctor will recommend further investigations into the underlying cause in order to formulate a treatment plan. Many cases of male infertility are treatable with lifestyle changes, medications, surgery, and other interventions.